30 Mar 2021 Walking on air
By John Patton
Doctors and nurses treating patients at Conway Regional Medical Center with congestive heart failure (CHF) now have a new tool to help provide accurate, timely care for the duration of their patient’s hospital stay. The best part for patients is that it is fast and does not cause discomfort.
This new portable device is giving physicians and nurses an advantage in diagnosing and treating CHF patients who come into the emergency department.
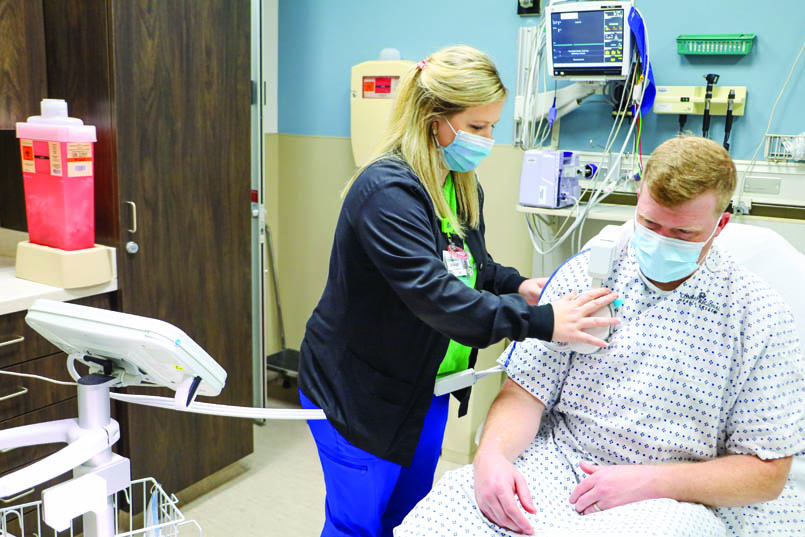
The Remote Dielectric Sensing (ReDS) system uses a noninvasive, radar–like technology to accurately determine the amount of fluid in a patient’s lungs. It can perform a test in approximately 90 seconds. Conway Regional is the first health system in Arkansas to use the device, according to the manufacturer, Sensible Medical.
Don Steely, MD, an interventional cardiologist with the Conway Regional Cardiovascular Clinic, noted that Conway Regional’s investment in the scanner is another instance in which the health system is growing to meet of the needs of the growing community.
Steely said the scanner is especially helpful in determining whether a patient has CHF or asthma. “If a patient comes into the ER experiencing shortness of breath, this is a more efficient, noninvasive way of measuring the amount of water in the lungs,” he said. “It reduces the need for invasive blood tests and X–rays.”
Steely explained that the device calculates the percentage of water in a patient’s lungs by measuring lung tissue density. The higher the density of the tissue, the larger the volume of water.
Steely said the ReDS lung scanner enables the staff to monitor the progress of CHF patients while they are in the hospital. While ReDS is not recommended in every situation, it can be a reliable system for many patients who are experiencing breathing issues.
Nurses’ Perspective
“We use ReDS on a weekly basis in the inpatient and outpatient settings,” said Amanda Irby, RN, Conway Regional’s Director of Emergency and Critical Care Services. “It helps us ensure our patients are being treated quickly and accurately, and it also helps us make sure the patient is ready for discharge at the appropriate time.”
JoLeigh Davidson, RN, in the emergency department, is one of the nurses who uses the lung scanner on a regular basis.
“It’s so helpful — it is great with our patients who have heart failure,” said Davidson. “Not only does it give us a percentage of how much fluid is in the lungs, it also provides a protocol that helps us plan care for the patient based on that percentage.”
Davidson describes the ReDS scanner as an extra tool that speeds up patient care.
“It’s very quick,” she said. “It fits on the outside of the chest, and we make sure it is positioned to get an accurate reading. It is not invasive at all.”
She also noted that it gives the staff the ability to quickly monitor the day–to–day care of patients with fluid buildup on their lungs. If the result is less than 20 percent, the patient may be dehydrated.
If the fluid percentage is in the normal range of 20 to 35 percent, basic lab tests or chest X–rays may be needed to determine why the patient is experiencing breathing issues. If the fluid percentage is 36 percent or higher, physicians may want to prescribe medication or take other medical action to reduce the fluid buildup.
Steely emphasized that by providing innovative tools such as the lung scanner, Conway Regional not only helps him diagnose and treat patients but also, “provides cutting–edge care with a heart.”











